Nephrotic Syndrome Signs and Symptoms Management Nursing Care It is a clinical state in which a group of symptoms that can be developed in many renal diseases. In which abnormal increased permeability to pass plasma proteins. Proteninuria increases and plasma proteins decrease.
The main characteristics of Nephrotic syndrome are edema, Proteninuria, hypolabunaemia; hypercholesteremia the cause is known resteraemia. Increased Permeability of the Glomerulus leading to loss pf Proteins in to the tubles
Classification Nephrotic Syndrome
(i) Minimal change Nephrotic syndrome.
(ii) Secondary Nephrotic syndrome
(iii) Congenital Nephrotic syndrome (usually die by second year of life).
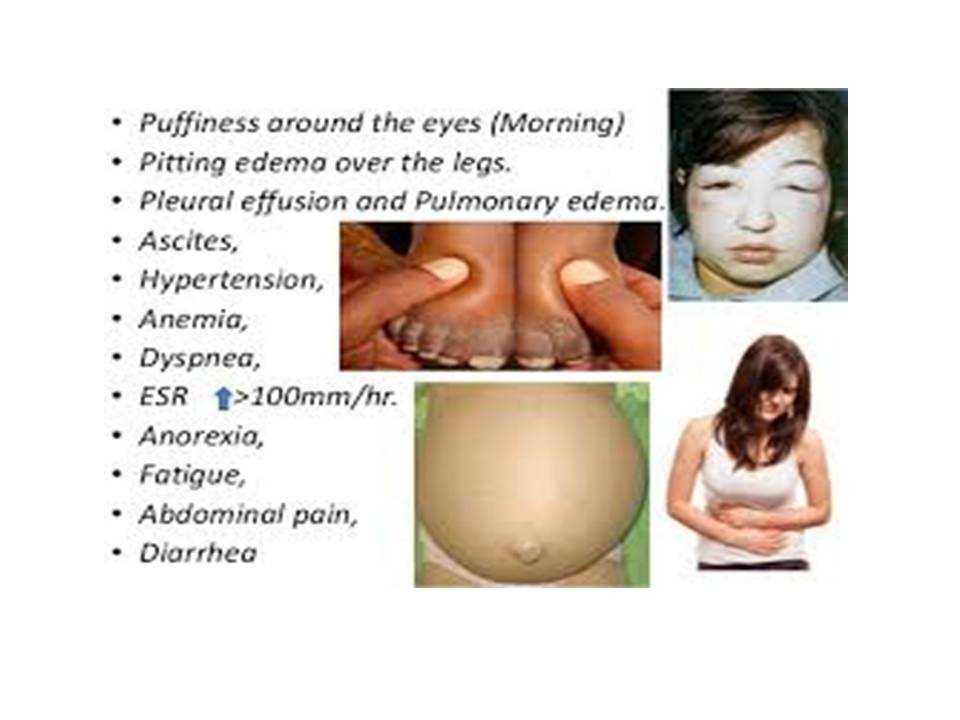
Signs and Symptoms of Nephrotic Syndrome
- Proteinuria
- Hypoalbumineamia, general health loss of appetitie.
- Hyperlipemia.
- Generalized dependent edema, especially genital, periorbital and abdominal (ascitis).
- Symptoms of nephritis hematuria and hypertension.
- Weight gain.
- Vomiting anorexia and diarrhea.
- Child becomes irritate & fatigued.
- Urine output decreases.
- Muscle wasting and pallor skin.
- Frothy Urine,
- Leukonychia,
- DVT – Deep Vein Thrombosis,
- MI- Mayocardial Ischemia,
- Leukonychia,
- Blood Pressure Normal or Raised,
- Generalized symptoms – Reduced appetite, Lethargy, Fatigue,
Cause for Nephritic Syndrome
- Primary Glomerulus Nephritis,
- Secondary Glomerulus Nephrotic Syndrome,
Secondary Glomerulus Nephrotic Syndrome Causes,
- Diabetic Nephropathy,
- Cancer,
- Vasculitis,
- Sarcodosis,
- Amyloidosis,
- Multiple Myeloma,
- Infections i,e. Hepatitis B, Syphylis, HIV,
- Drugs i,e NSAIDs, Pencilamine, Gold, Captopil,
Nephrotic Syndrome Pathophysiology
Diagnostic Evaluations for Nephrotic Syndrome
- Urine analysis for proteins, casts and specific gravity.
- Blood for total serum protein and albumin and globulin levels.
- Erythrocyte sedimentation rate.
- Serum cholesterol.
- Immmunoglobulin,
- Electrophorosis,
- Renal Ultra Sound,
- Renal Biopsy in Audults,
Nephrotic Syndrome Treatment: Conservative Therapy,
- Monitor Urine Output and Urine Examination,
- Blood Pressure Monitoring,
- Fluid and Electrolyte Balance,
- Weight,
Medical Managemnt for Nephrotic Syndrome:
- Diuretics,
- ACE- Inhibitor,
- Cortico Steroids / Immuno Suppresents,
Supportive therapy is given
- Salt restricted diet is given.
- Corticosteroid therapy are given for 4 weeks & response to therapy usually takes within 7 to 21 days.
- However the dose of gradually discontinue when satisfactory response is noted.
- Immuno suppressant therapy for children who do not respond to steroids or those who have frequent relapses eg: chlorambucil (Leukean), cyclo sporine (sand immune), cyclophosphamide (cytoxan).
- Diuretics are used to relieve oedema in severe anasarca.
- Antibiotics are used to treat the infection.
- Abodminal paracentesis is done to relieve thepressure in case of breathlessness.
Nephrotic Syndrome Surgical Management
- Renal Transplant,
Nephrotic Syndrome Nursing Care
- Assess the vital signs of Blood pressure and monitor them frequently.
- Maintain fluid balance and the requirement is calculated according to the output and weight of the child.
- Record the daily weight and it whould be compared with oedema and output which should be done daily.
- Daily urine examination is done for specific gravity and albumin.
- Measure the abdominal girth daily to assess the oedema.
- The diet should be low in sodium and high in proteins.
- The Dyspnea due to ascitis is relieved by sitting position and abdominal paracentesis to relieve upward pressure on the diaphragm.
- Observation of early signs of infection is necessary as both disease state and drug therapy increases the susceptibility. Thus the child should be protected from others who are ill. Teach the parents the signs of impending infection and encourage them to seek medical care.
- Malnutrition caused by loss of proteins and poor appetite, so the child should take diet containing high protein. For example eggs, milk, pulses, soya bean and groundnuts and restrict the fluids if ordered.
- Proteins may be given 4 to 5 g / kg of body weight according to serum protein levels and tolerance of the patient.
- Adequate calories should be supplied. Feeds may be small & frequent.
- Encourage the patient in Fowler’s position to decrease pressure against diaphragm, as the patient has respiratory difficulty caused by ascitis.
- Care of the oedematous skin must be done by positioning and by giving skin care and cleaning and keeping the skin dry. Powder may be applied and in male child having oedematous scrotum, the scrotal support is required with ‘T’ bandage to prevent friction.
- Explain and educate the child and provide psychological support as the child would be disturbed due to body image disturbance.
- Encourage the child to participate in own care.
- Help the parents to understand that mood swings are influenced by physical condition.
- Encourage for divisional activities that provide satisfaction.
Parental Advice:
- Explain the parents about the need of follow up and risk of relapse.
- Emphasize on high protein diet.
- Demonstrate urine test for albumin.
- Explain about administration of the medicine and its continuation.
- The maintenance of the medicine and its continuation.
- The maintenance dose should be explained which may be over 8 to 12 months period.
- Parents should be told about the side effects such as Cushing O aid appearance, gastro intestinal bleeding sodium retention and hypokalemia.
Nephrotic Syndrome Complications: Immuno suppressive therapy resulting in recurrent infection.
- Hyper coagulability.
- Urinary infection,
- Pleural Effusion,
- Ascities,
- Thrombosis,
- General Oedema,
- Recurrent Infections,
- Growth retradations,
- Calcium & Vitamin D Deficiency,
- Protein Energy Malnutrition,